ATV accident claims 12 year-old’s life

Bluewater Health poised to help nursing homes in second wave
October 14, 2020
Heather Wright/The Independent
Officials at Bluewater Health say they’ve worked through the summer with long term care homes to prepare them for a second wave of COVID-19.
This as Ontario’s Patient Ombudsman called for immediate action in long term care to prevent more deaths during the second wave of the pandemic. Cathy Fooks released an interim report recently after getting a large number of complaints about how long term care homes were handling the COVID-19 pandemic.
Families, residents and staff at homes across the province called the office worried about loved ones in homes. “We received over 100 complaints about infection prevention and control in long-term care homes,” wrote Fooks.
“Caregivers also expressed concerns about lack of communication from hospitals and long-term care homes. Given their inability to visit, caregivers told us that the lack of communication is particularly distressing.”
And, many of the complaints were about significant problems jeopardizing the safety of staff and residents. The situation was so dire that Fooks contacted the Minister of Long Term Care in both April and May to express her concerns and explain some of the major issues.
Patient Ombudsman also started active investigations to try to fix problems which were directly hurting residents and the staff, including in homes where the shortage of personal protective equipment was leading to personal support workers becoming ill.
Fooks says “every long-term care home should have a partner organization to provide support for management, infection prevention and control, and staffing to prevent and respond to any COVID-19 outbreaks.”
Julia Oosterman, the chief of communications at Bluewater Health, says “this is happening informally in Lambton already.”
In May, when Vision Nursing Home spent weeks in outbreak with 10 people dying, Bluewater Health came along side the home and worked on infection control and the use of personal protective equipment. Eventually, some residents were transferred to hospital so the home could undergo a deep cleaning.
And while the Patient Ombudsman is asking for a formal link, Oosterman says the hospital has already been reaching out to homes to help with any ongoing concerns about infection control.
“We’ve reached out to many of the homes in the community…because the minute an outbreak happens, the hospital will be affected. We need to figure out how to keep people safe in place so, as much as it is possible, we not have outbreaks and we do not have 15 to 20 people coming to hospital.”
Oosterman expects if long term care homes are affected in Lambton, they will be better prepared simply because we know more about how the virus spreads.
Aside from hospital support, Fooks also urged the government to make sure essential caregivers remain by residents sides, with proper infection control measures.
“Visitor restrictions based on the recommendation and at the direction of the Chief Medical Officer of Health have undeniably been a significant hardship on patients, residents and their families,” she said, adding many family members could not make decisions on care for their loved ones because they couldn’t enter the home.
Fooks said they heard accounts of long term care home residents and patients dying alone without their families there to support them. “Many of the people who came to our office reported that they meet the definition of an “essential visitor”, and did not understand why they were not able to visit or accompany family members who need support to receive health care.”
The province has already changed the rules to allow caregivers to be by the family’s side even during an outbreak. However some senior’s advocates are worried that recently Dr. Barbara Yaffe, Ontario’s Associate Chief Medical Officer of Health said local public health officials could stop essential care givers from entering into homes during an outbreak situation.
Fooks says long term care homes also have to do a better job communicating with the residents and their families.
Fooks also wanted whistle blower protections enhanced for workers. She says they received 20 whistle blower complaints from April to June and many were of a “very serious nature” in long term care homes.
Some were about residents not receiving basic care because there simply wasn’t enough staff on site.
NEXT
Another Lambton resident tests positive for COVID-19
PREVIOUS
Corunna parents told of COVID-19 case in local public school

ATV accident claims 12 year-old’s life
July 9, 2025
Read More
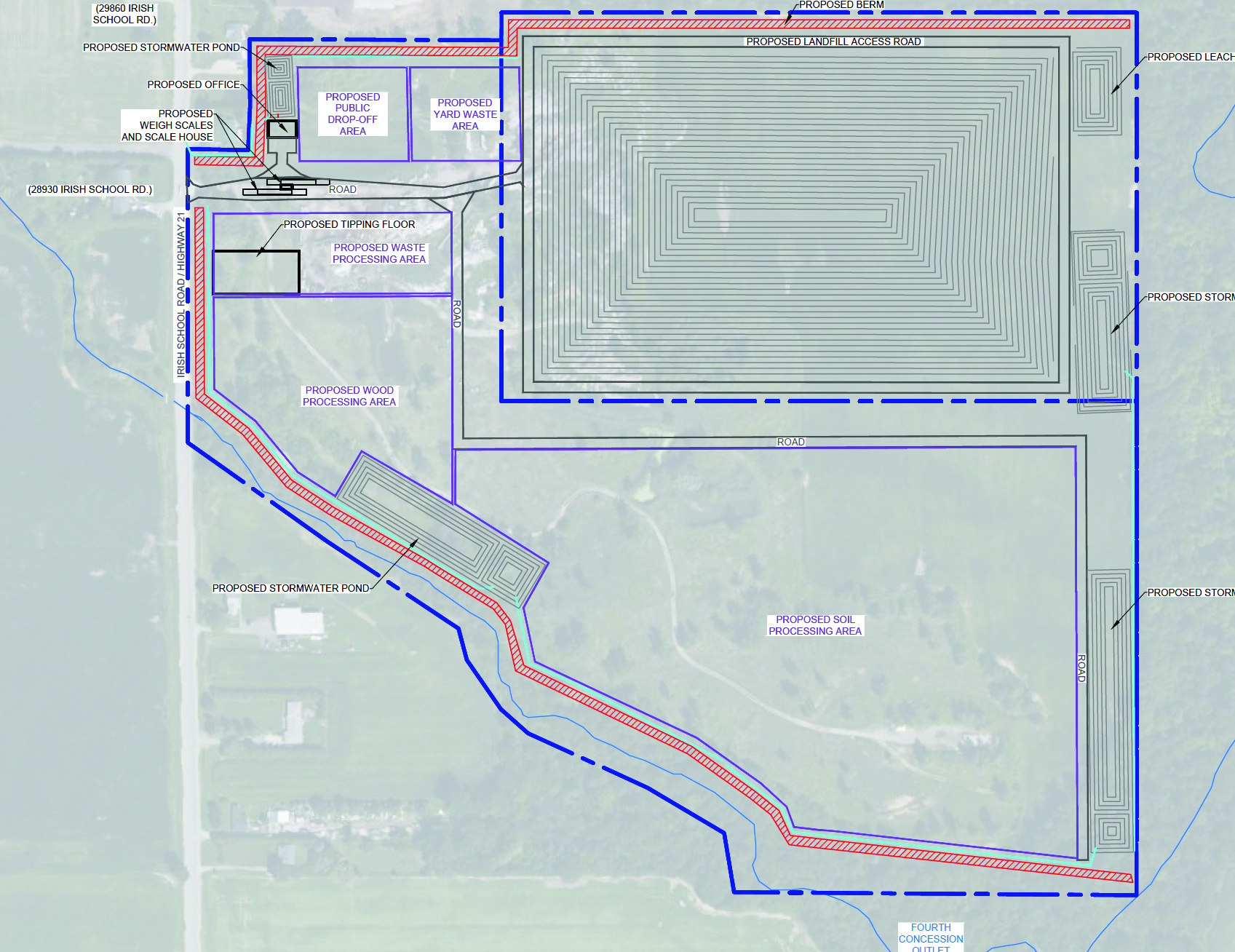
Conservation authority voices water concerns at York1 site
July 8, 2025
Read More

$1M grant to upgrade Moore Sportsplex
July 8, 2025
Read More

Private paid Ipperwash parking OKed
July 8, 2025
Read More
